Overview

Your foot is made up of 26 bones, 33 joints, and more than 100 tendons. The heel is the largest bone in your foot. If you overuse or injure your heel, you may experience Heel Pain. This can range from mild to disabling. In many cases, if you have heel pain, you will need a doctor to diagnose the cause.
Causes
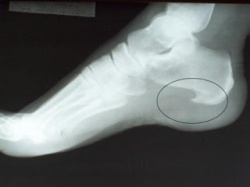
While heel pain has many causes, it is usually the result of faulty biomechanics (abnormalities in the way we walk). This can place too much stress on the heel bone and the soft tissues attached to it. The stress may also result from injury, or a bruise incurred while walking, running or jumping on hard surfaces; wearing poorly constructed footwear; or being significantly overweight. Systemic diseases such as arthritis and diabetes can also contribute to heel pain. A common cause of heel pain is the heel spur, a bony growth under the heel bone. There are no visible features on the heel, but a deep painful spot can be found in or around the middle of the sole of the heel (see diagram). Approximately 10 per cent of the population may have heel spurs without any pain. Heel spurs result from strain on the muscles of the foot. This may result from biomechanical imbalance, a condition occurring in many people. Both heel pain and heel spurs are frequently associated with an inflammation of the long band of tissue that connects the heel and the ball of the foot. The inflammation of this arch area is called plantar fasciitis. The inflammation may be aggravated by shoes that lack appropriate support, especially in the arch area, and by the chronic irritation that sometimes accompanies an athletic lifestyle.Excessive rolling in of the feet when walking. An inflamed bursa (bursitis), a small, irritated sack of fluid at the back of the heel. A neuroma (a nerve growth). Other soft-tissue growths. Heel bumps or ?pump bumps?, a bone enlargement at the back of the heel bone. Bruises or stress fractures to the heel bone.
Symptoms
Sever?s Disease. This is a condition that occurs in 10 – 15 year old children, predominantly boys and is associated with running and repetitive jumping. It is also associated with flimsy footwear that kids may wear. It occurs when the Achilles tendon continually pulls on the apophysis of the calcaneum and does not allow for it to fuse with the body of the calcaneum. Calcaneal enthesopathy. This occurs when there is repetitive trauma at the attachment of the Achilles tendon, resulting in a spur from the calcaneum up into the Achilles tendon. It is usually visualized on x-ray and may be tender if there is an associated bursitis or tendonitis. “Pump Bump”. Also known as Haglund?s Deformity, this is a bony enlargement that exists on the back of the heel – usually related to a congenital abnormality or with chronic bursitis, causing a thickening. There may have already been trauma or pressure from footwear. Treatment is usually protection of the bump and correct footwear. Associated with a symmetrical swelling at the base of the Achilles tendon. It is usually related to repetitive trauma or inappropriate footwear. It is often red and hot in the early stages. Treatment is usually to correct the footwear, provide padding and treat the local symptoms e.g. ice, rest, physiotherapy and cortisone injection. Fat Pad Syndrome. Direct contact with the base of the heel may result in trauma to the fat pad. Related to obesity, training on hard surfaces, uneven grounds, poor shoes especially overlarge shoes which can cause shearing forces on the heel. These conditions are renowned for taking a long time to recover – usually many months.
Diagnosis
The diagnosis of plantar fasciitis is generally made during the history and physical examination. There are several conditions that can cause heel pain, and plantar fasciitis must be distinguished from these conditions. Pain can be referred to the heel and foot from other areas of the body such as the low back, hip, knee, and/or ankle. Special tests to challenge these areas are performed to help confirm the problem is truly coming from the plantar fascia. An X-ray may be ordered to rule out a stress fracture of the heel bone and to see if a bone spur is present that is large enough to cause problems. Other helpful imaging studies include bone scans, MRI, and ultrasound. Ultrasonographic exam may be favored as it is quick, less expensive, and does not expose you to radiation. Laboratory investigation may be necessary in some cases to rule out a systemic illness causing the heel pain, such as rheumatoid arthritis, Reiter’s syndrome, or ankylosing spondylitis. These are diseases that affect the entire body but may show up at first as pain in the heel.
Non Surgical Treatment
As heel pain is basically a stress problem in the tissues of the heel, the main treatment is to reduce stress. Your doctor will advise you about weight loss and appropriate footwear. A soft heel pad is useful to wear in your shoe to act as a shock-absorber when you walk. If you have a stiff ankle or tight Achilles tendon a physiotherapist can advise on exercises for these. Stretching the Achilles tendon and plantar fascia is very effective general treatment for many patients. If you have a high-arched or flat foot, a podiatrist may advise an insole to reduce stress. Simple pain-killers such as paracetamol or anti-inflammatory medicines can help reduce the pain. Ask advice from your doctor or pharmacist before taking anti-inflammatory medicines as they can have troublesome side-effects in some people. The simple measures above will help the majority of people with heel pain. If the pain continues, a splint to wear on your ankle at night to prevent your Achilles tendon tightening up while you are asleep is often very effective in improving the severe pain that many people get first thing in the morning and breaking the cycle of pain. Your GP or an orthopaedic foot and ankle surgeon or rheumatologist may inject some steroid into the attachment of the plantar fascia to damp down the inflammation. These measures will reduce the pain in most people who are not helped by simple treatment. If you still have pain after one or two injections, your doctor may want to investigate your problem a bit further. If no other medical problem or cause of stress in your heel is found, a number of other treatments can be tried. Further physiotherapy, wearing a plaster cast to rest the inflamed tissues, pain control treatments such as transcutaneous nerve stimulation (TENS) or acupuncture. Only if all non-surgical treatments fail would an operation be considered.
Surgical Treatment
With the advancements in technology and treatments, if you do need to have surgery for the heel, it is very minimal incision that?s done. And the nice thing is your recovery period is short and you should be able to bear weight right after the surgery. This means you can get back to your weekly routine in just a few weeks. Recovery is a lot different than it used to be and a lot of it is because of doing a minimal incision and decreasing trauma to soft tissues, as well as even the bone. So if you need surgery, then your recovery period is pretty quick.
Prevention

You can reduce the risk of heel pain in many ways, including. Wear shoes that fit you properly with a firm fastening, such as laces. Choose shoes with shock-absorbent soles and supportive heels. Repair or throw out any shoes that have worn heels. Always warm up and cool down when exercising or playing sport, include plenty of slow, sustained stretches. If necessary, your podiatrist will show you how to tape or strap your feet to help support the muscles and ligaments. Shoe inserts (orthoses) professionally fitted by your podiatrist can help support your feet in the long term.
A Morton’s neuroma is a benign (noncancerous) swelling along a nerve in the foot that carries sensations from the toes. The reason the nerve starts to swell is unknown. But once swelling begins, the nearby bones and ligaments put pressure on the nerve, causing more irritation and inflammation. This produces burning pain, numbness, tingling and other abnormal sensations in the toes. A Morton’s neuroma also is called an interdigital neuroma, intermetatarsal neuroma or a forefoot neuroma.



 Overview
Overview Symptoms
Symptoms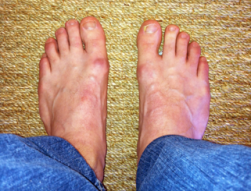






You must be logged in to post a comment.